Pediatric Orthopedic
physical Children are not young adults – Mercer Rang
Children’s bone are different from adult
Why you need Pediatric Orthopedic Surgeon?
Children’s musculoskeletal system is different from adults. They behave differently. Children have more capacity of remodeling & adaptation to environment. Their problem / disability can increase/ decrease/ static with the growth depending upon treatment and environment.
Their response to injuries, infection & deformities is quite different than adult. so approach of management in children is different from adults. They need specialized care.
Nowadays pediatric orthopedic surgery has become one of well-known subspecialty and training in this field is different from general orthopedic surgeon.
Pediatric orthopedic surgeon gets initial training in general orthopedics to treat general orthopedic problems and then gets specialized in pediatric orthopedics to treat musculoskeletal problem in children up-to the age of 19 years.
Pediatric orthopedic problems range from congenital bony abnormality of bone like Club Foot (CTEV), congenital hip dislocation (CDH), congenital dislocation of knee (CDK), Congenital Limb Deficiency and muscles to developmental problems like Rickets, Cerebral Palsy, Infection of bone and injury and Arthritis.
Neglect and improper management of these problems can lead to persistent physical disability that continues in adult. Indirectly it affects whole family and leads to psychological and financial burden.
How bones are Different in Children Than Adult?
- In small kids, some of the bones have many ossification centers as cartilage. So it looks like that they have more number of bones in body (300 in new born , some of them in cartilaginous mass ) but as they grow these centers fuse with the primary bone in adults (206 bones in adults )
- Children’s bone are in growing phase. They grow in length by the physical growth plate (cartilaginous plate on both end of bone) & in width through bone deposition on surface by appositional (periosteal) growth.
- As the child grows, bones in body remodel and realign according to need and specific pattern of development. But if injury affects growth plate and they fuse partially or completely then limb deformity / shortening can develop as they grow.
- Children bones are more flexible than adult bones and have thick periosteum, so their bones are more prone to deform / buckling /incomplete/ minimally displace fracture.
- Children bones heals faster than adults, can remodel and reshape easily. Younger the age, better the remodeling potential. So most preferably injuries can be managed by plaster and observation. But some bones in body like hip & elbow fracture are more likely to create trouble so they need surgery to fix it. Injury to long bones in children can stimulate excessive growth that lead little lengthening so little shortening after union of bone can be accepted.
- Children are more active and mobile and it is difficult to control their mobility, so they need more supervised treatment under the care of parents.
- Kid’s ligaments are stronger than bones so they brake the bone through physical growth plate more easily as compared to ligament sprain or rupture.
- Some of the normal variant in development process can be mistaken as pathology so we have to be very cautious.
- Etiology and pattern of pathology of different problems are totally different than adults and even different in different age.
- High risk of musculoskeletal injury in early phase of puberty due growth spurt. Lot of changes in biomechanical property of bones and muscles occurs in this age. It creates imbalance in strength and flexibility.
- Children’s bones are smaller and have faster union rate than adults so they need different implant and fixation system than adults. Bone injury in very small kids heal by lot of new bone so some time these are mistaken as different pathology.
- Bone end in joint of children are covered / made by very thick soft cartilage so these are more prone to damage and absorption by joint infection and lead to long term complications of joint deformity, dislocation and limb length discrepancy etc. So they need urgent surgery to drain the pus. In adults these coverings are by thin layered cartilage.
- Secondary ossification centers appear at different ages, so age determination is being done on the basis of these ossification centers appearance and disappearance.
- Cartilaginous growth plate and bone end are not visible on X-ray so in affection of cartilage we need ultrasound/ MRI and sometime arthrogram (X-ray after contrast dye in joint ).
- Every child progress in specific developmental milestone with very small variation. If child deflect in major ways from this developmental milestone pattern then they can have some growth abnormality like cerebral palsy, down syndrome etc.
- Some children with some specific diseases affecting bones are advised not to participate in sports activities. These diseases are osteogenesis imperfecta, Vitamin D resistant rickets, rheumatoid arthritis, upper cervical anomalies like antlantoaxial instability.
Club foot (CTEV ) –
Club footis also known as congenital talipes Equinovarus. It is a complex, congenital deformity of foot, in which one or both foot is rotated & twisted inward. It is complex deformity of foot involving muscle, ligament and bone of whole feet and ankle. Treatment of club foot can be started any time after birth. Early the treatment, better is the outcome. It can be positional, idiopathic & syndromic. Idiopathic variety is the commons. Syndromic variety is the part of some syndrome and very rigid deformity, less amenable to treatment with high recurrence.
Treatment for CTEV :
No treatment for positional club foot
Idiopathic- 4-5 plaster by Ponsetty technique at 10 days interval then TA tenotomy & plaster for 1 months followed by CTEV denise Browne brace & foot stimulation, stretching for 1-1.5 year. Early the application of plaster even in 1 week of delivery give better outcome.
Syndromic Club feet- Ponsetty plaster 5-8 time followed by tenotomy and brace. Sometime surgery may be required. Long term use of brace is required. Child may need repeated plaster application.
Methods of treatment in recurrence / neglected deformity-
- PMSTR- soft tissue surgery. Nowadays it is rarely needed but some time part of this procedure is needed
- Tendon transfer- to balance the muscle imbalance in older age after 5 year of age.
- Double osteotomy- it is kind of bony surgery in which medial border of foot is lengthen and lateral border is shorten
- Tendon lengthening- tendon lengthening can be associated with any other procedure to get results.
- Ilizarov/ JESS fixater- in neglected/ recurrent/ rigid/previously operated cases
Congenital Vertical Talus (CVT)-
Rare congenital anomaly of foot in which talus bone in ankle pointed toward vertically in place of parallel to ground. It present as an extreme cases of flatfoot. Usually it is sever deformity of foot. mild variety is oblique talus deformity.
Treatment Congenital Vertical Talus:
Manipulation and plaster application by reverse ponsetty technique for 5-6 time followed by surgery on foot and plaster. Brace will be given for few months. In neglected cases, surgery will be required to correct the deformity.
Flat foot-
Flat feet is normal in babies & toddlers. Babies are often born with flat feet. Most of time children have fat pad on the inner border of their feet that hides the arch. Their muscle and ligaments are more flexible, so when they stand their arch flatten. Flat feet usually resolve by the age of 6 years of age as the longitudinal arches develop. 10% of flat feet persist even in adult.
Treatment For Flat Foot:
Active treatment is needed except reassurance, bare foot walking. Foot insert like arch support should not be prescribed.
Treatment is required in painful symptomatic cases which usually occur because of some other associated reason like vertical talus, tarsal coalition, arthritis etc.
Congenital Dislocation of Hip/ Developmental Dysplasia of Hip (CDH/ DDH):
It is the disorder of abnormal development of hip joint resulting in acetabular dysplasia (underdeveloped roof of hip joint)/ subluxation ( incomplete dislocation)/ complete dislocation of hip. This problem is being diagnosed by the clinical examination and radiological investigation like x-ray and ultrasound
Treatment for CDH/DDH:
0-6 months of age
Pavlik harness- it is a kind of brace that keep the femoral head inside the joint. This brace should be wear 24 hours in a day till the hip became stable. This brace can only use till the age of 6 months of age.
6months to 1 year of age
Close reduction & hip spica- hip dislocation will be reduced under anesthesia and double hip spica will be applied. Arthrogram can be done to confirm the congruency of joint.
9 months to 18 months:
Open reduction: joint will be reduced by the surgery and hip spica will be given.
1.5 year onward:
Open reduction & femoral shortening: if reduction is difficult, the bone shortening of thigh is required to reduce the joint. This shortening is usually recovered due to growth stimulation.
Acetabular reconstruction: Acetabular reconstruction is required if socket of hip joint is not well formed. Usually done in children after the age of 18 months.
Congenital dislocation of knee/ hyperextension of knee (CDK):
Usually this problem arise when new born with breech delivery, or have some genetic disorder like AMC. Tibia is dislocated anterior to knee joint and you cant bend the knee. Easily diagnosed at time of birth.
Treatment for CDK:
- Non-syndromic variety can be managed successfully with the manipulation and plaster application
- Surgery is required in severe variety.
- Precut quadriceps tenotomy
- Quadriceps lengthening
- Bone shortening
Septic Arthritis (infection of joint) –
It means collection of pus inside joint. Neonatal septic arthritis should be taken as septicemia.
Septic arthritic in neonate need urgent attention. Infant will be failure thrive, fever, pain, inability to move joint and extremity etc. investigation like blood investigation, ultrasound and x-ray of hip is required.
Bone end of the long are covered with thick cartilage and they are more prone to damage by the inflammatory cells present in pus. So early drainage of pus by surgery, intravenous antibiotic is required.
Osteomyelitis (bone infection):
Infection of bone in children can cause lots of disability in long term. Child will have high grade of fever, inability to use extremity, pain, swelling, redness in affected part.
In acute case before the formation of pus can be managed by IV Antibiotics, after 48 hours they need surgery to drain pus inside the bone. Long persistent infection of bone can damage the bone in variable degree depending upon extent of involvement, age, immunity, treatment.
In these cases surgery is required to drain the pus and dead bone has to be removed. If bone is damaged too much then reconstruction of bone and joint is required.
Congenital hip dislocation
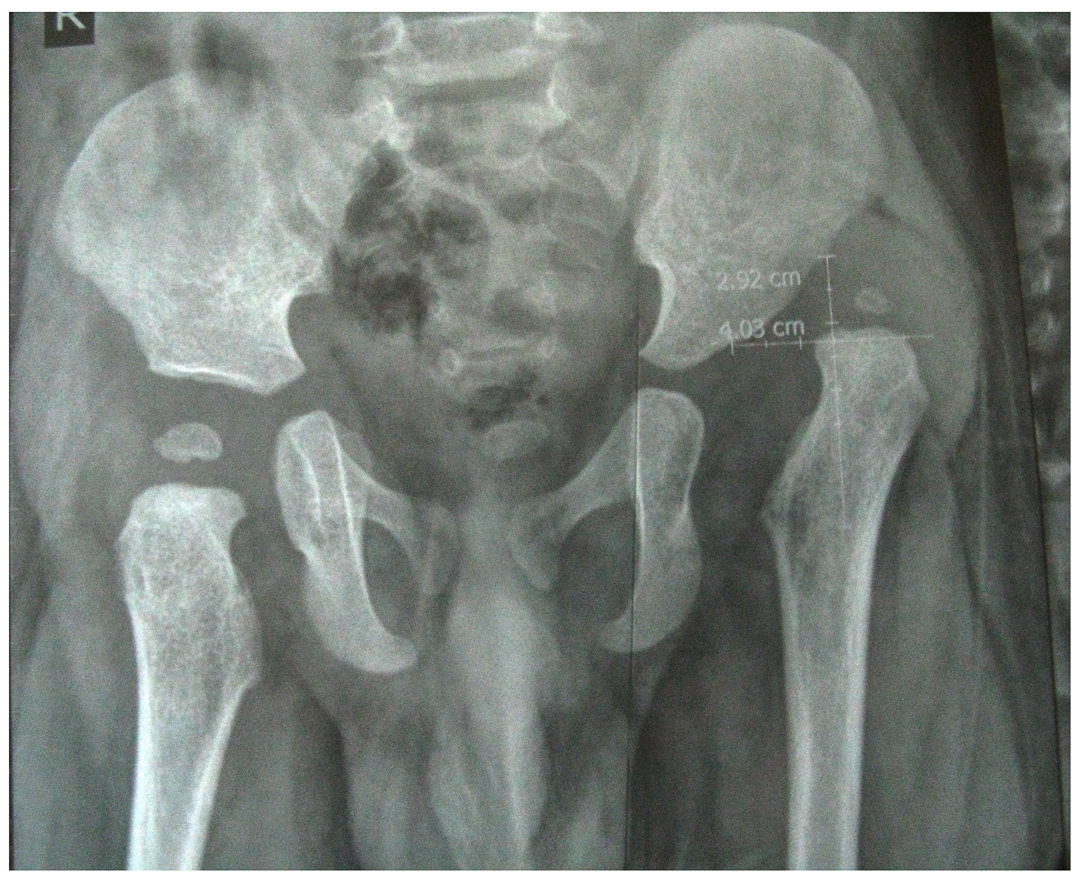
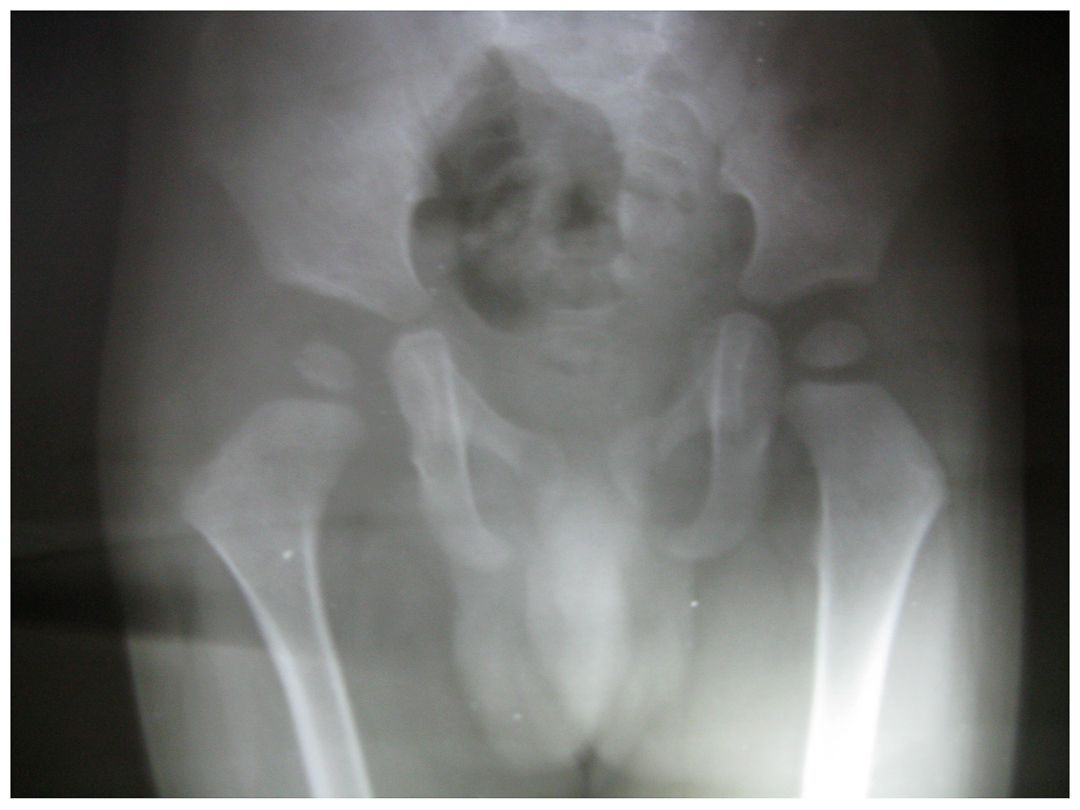
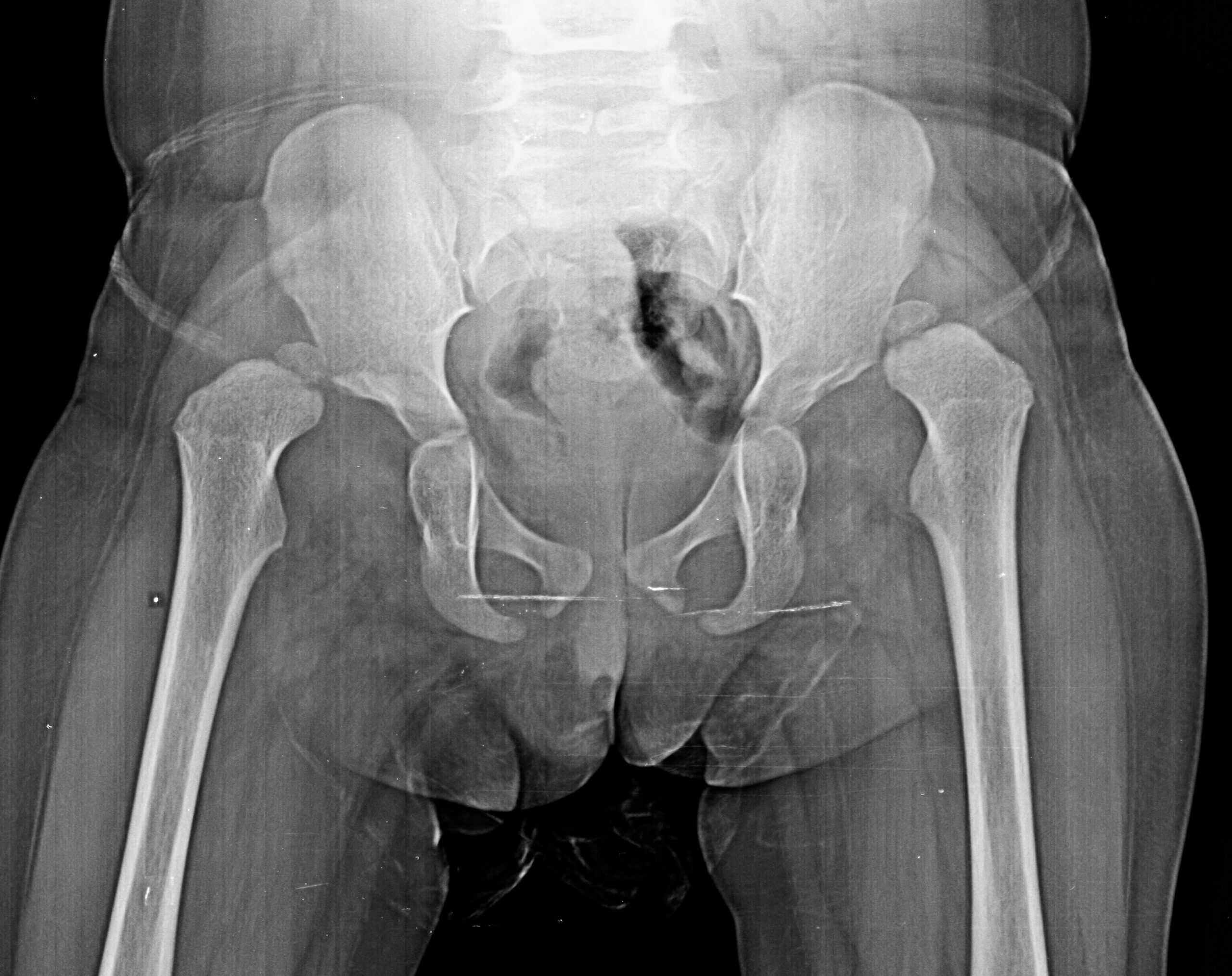
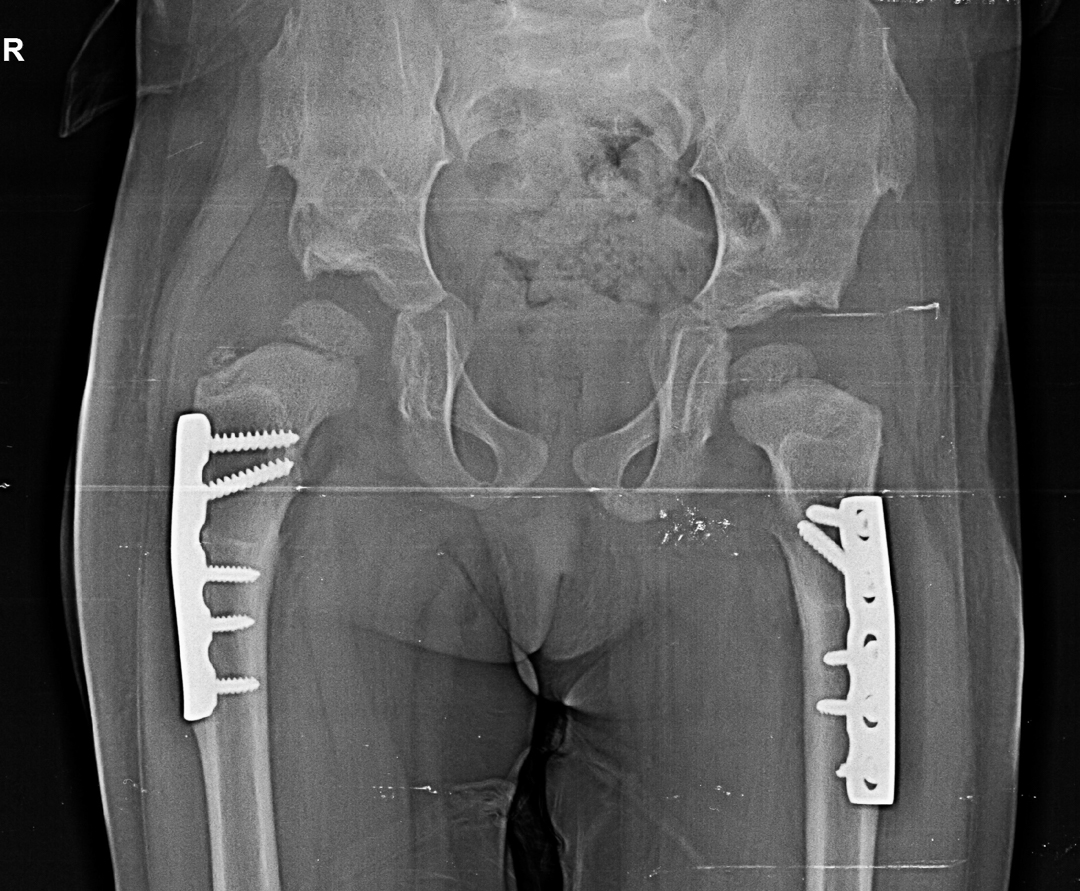
CTEV (club foot )
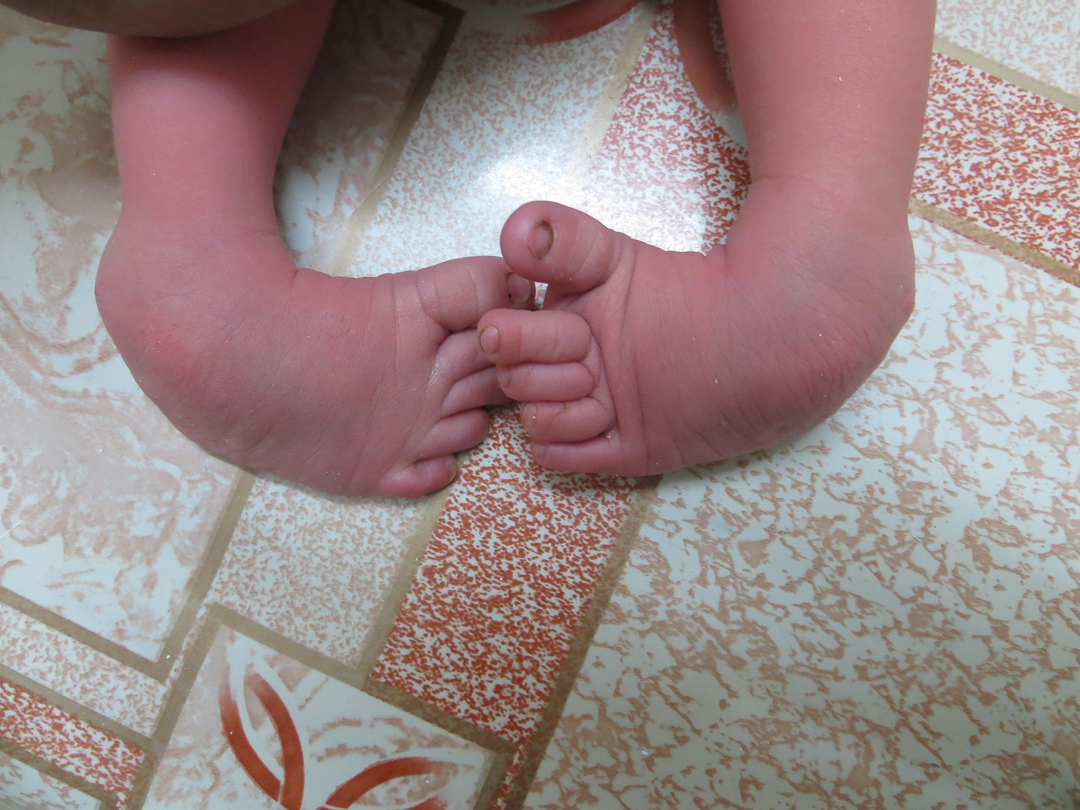
Before

After
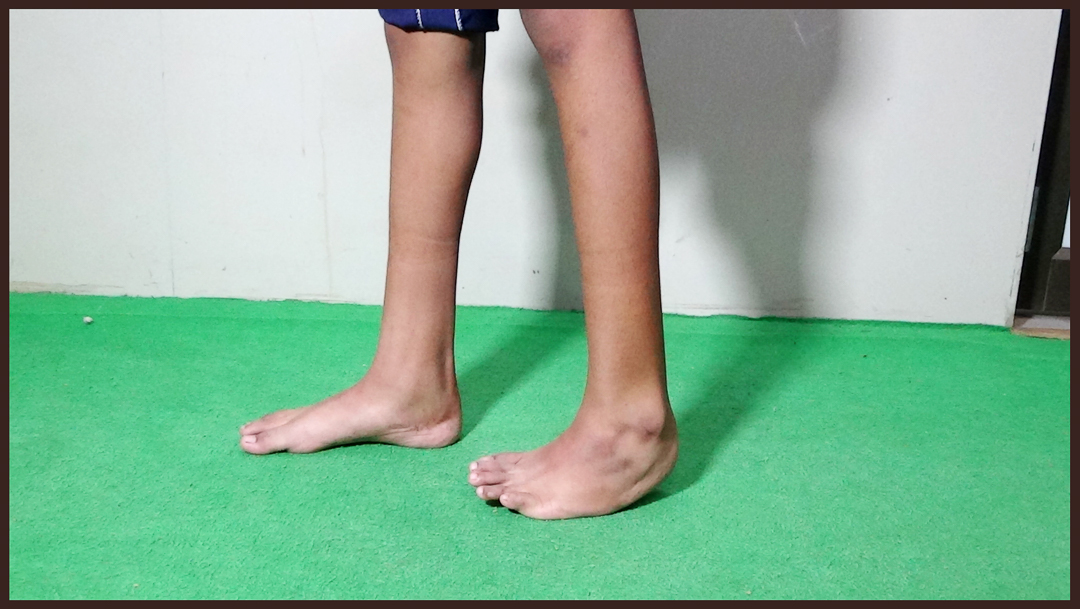
Before
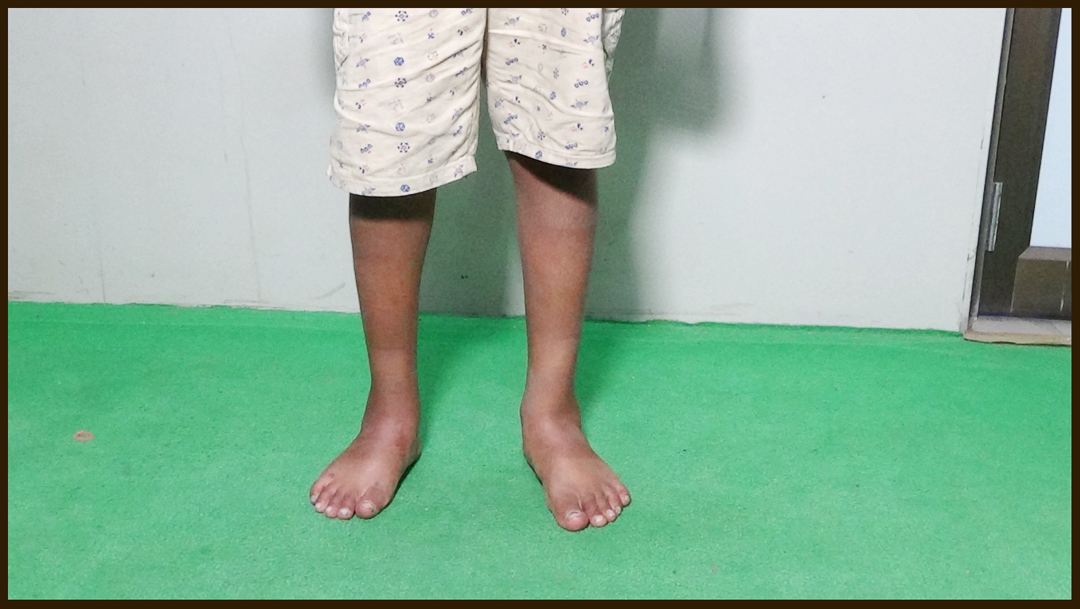
After
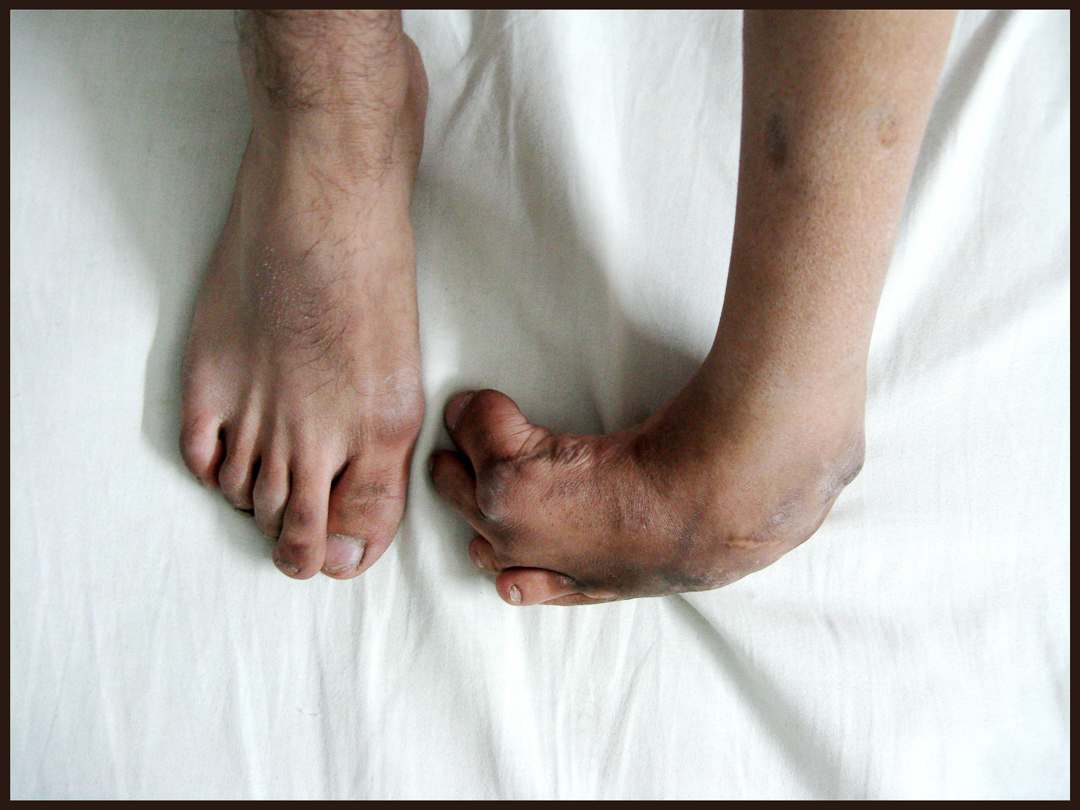
Before
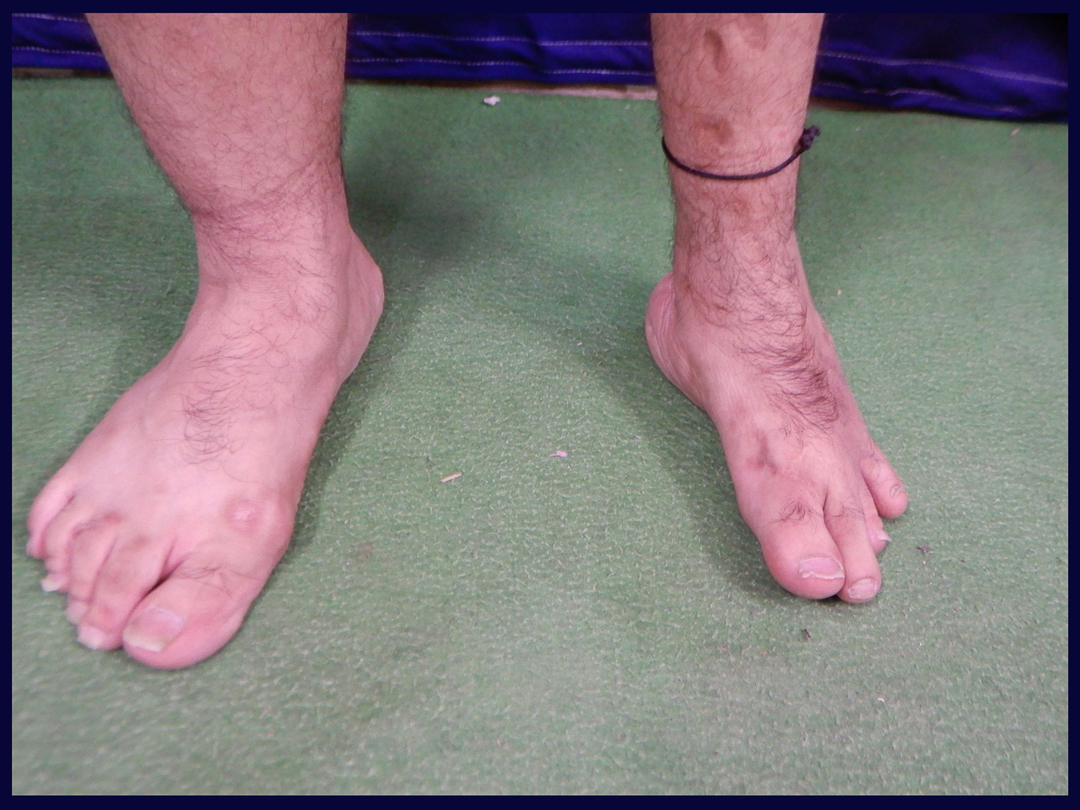
After
Osteomyelitis radius with bone loss
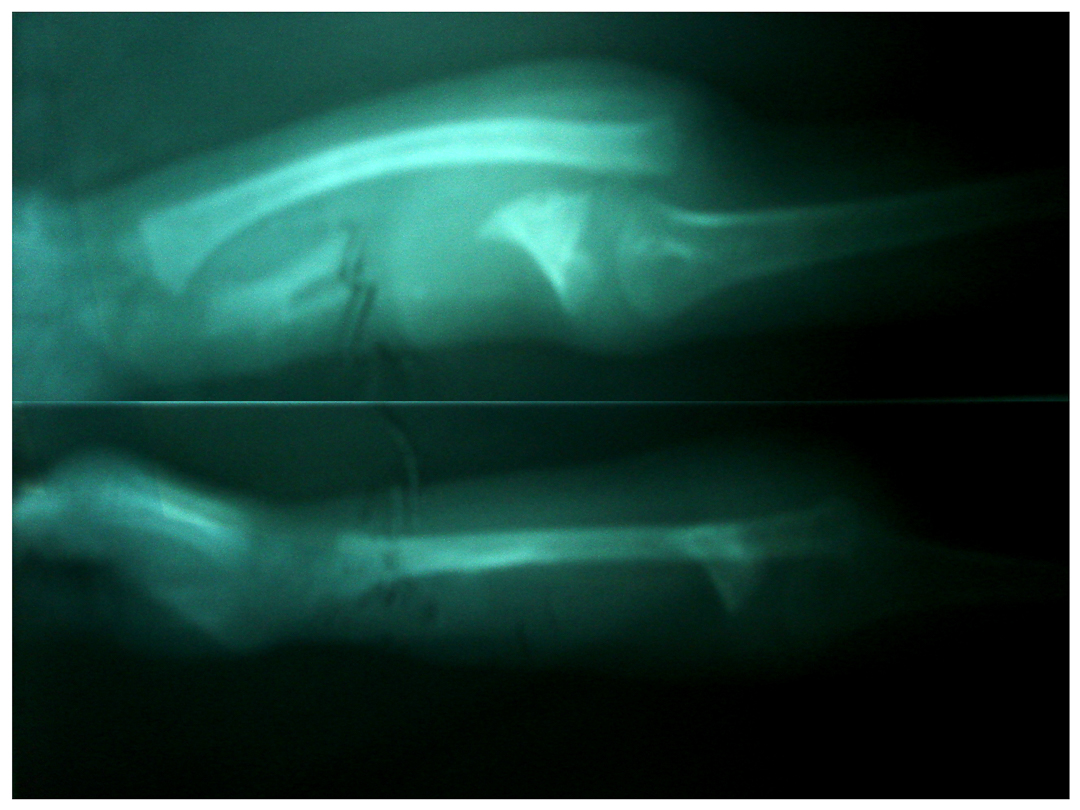
Before
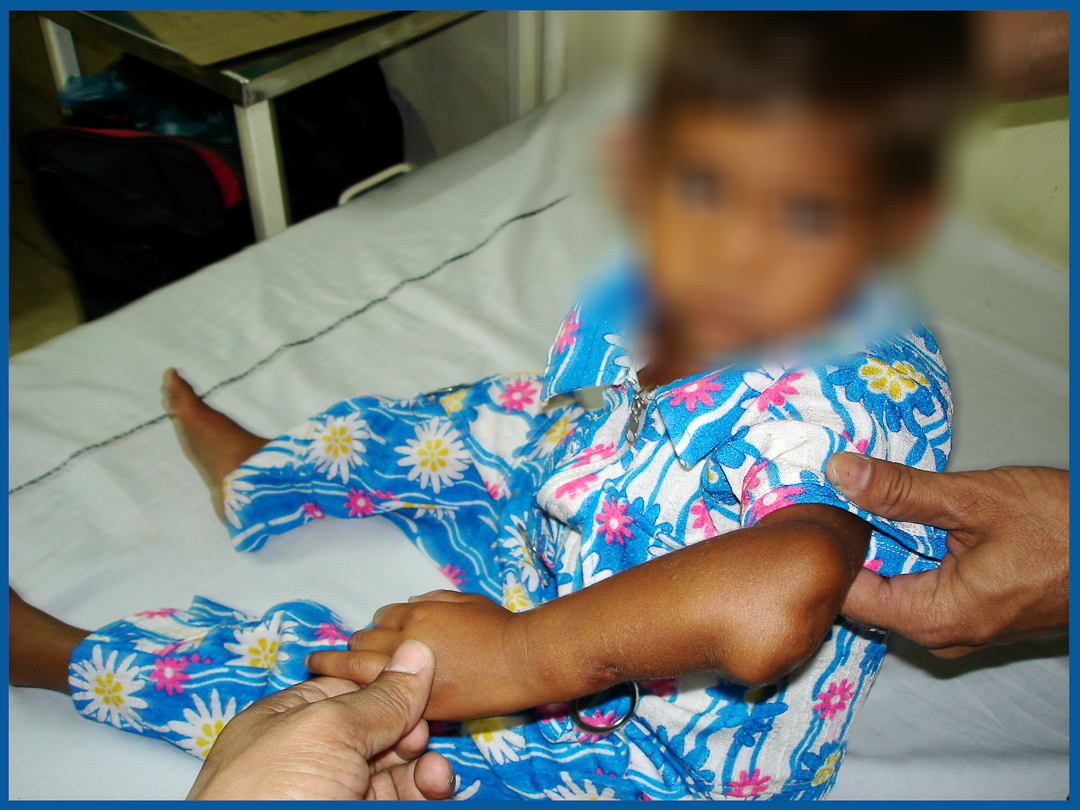
Before
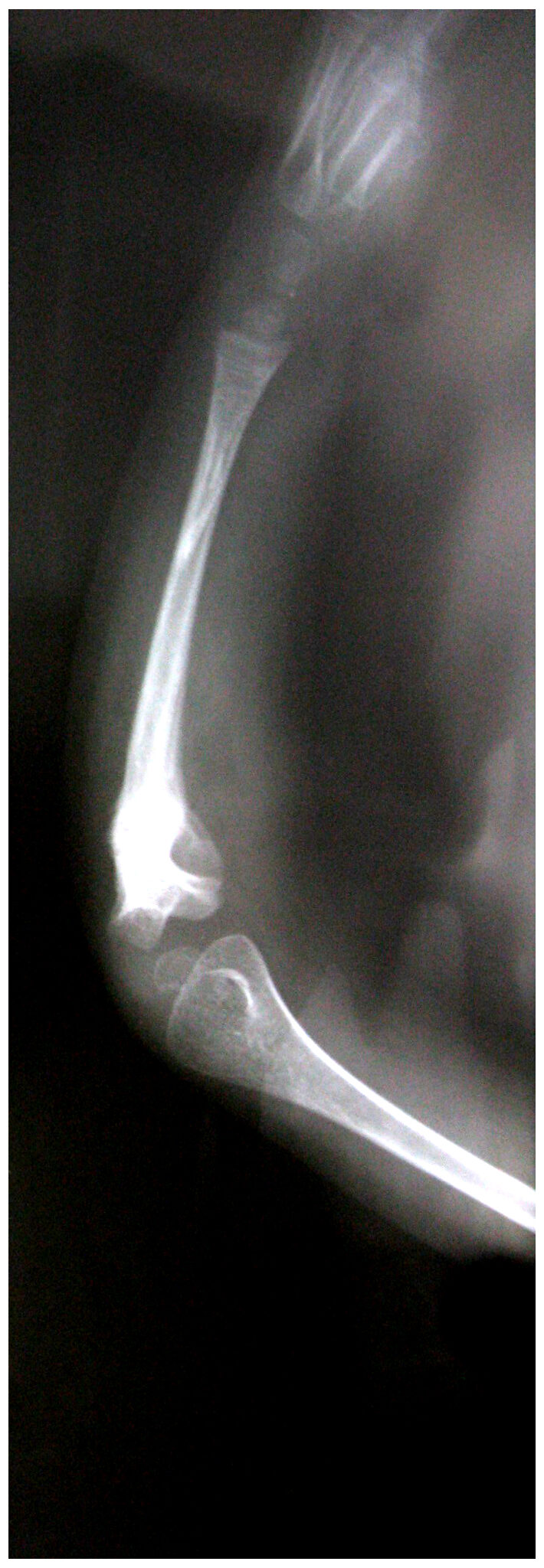
After

After
Osteomyelitis dista tibia & femoral neck
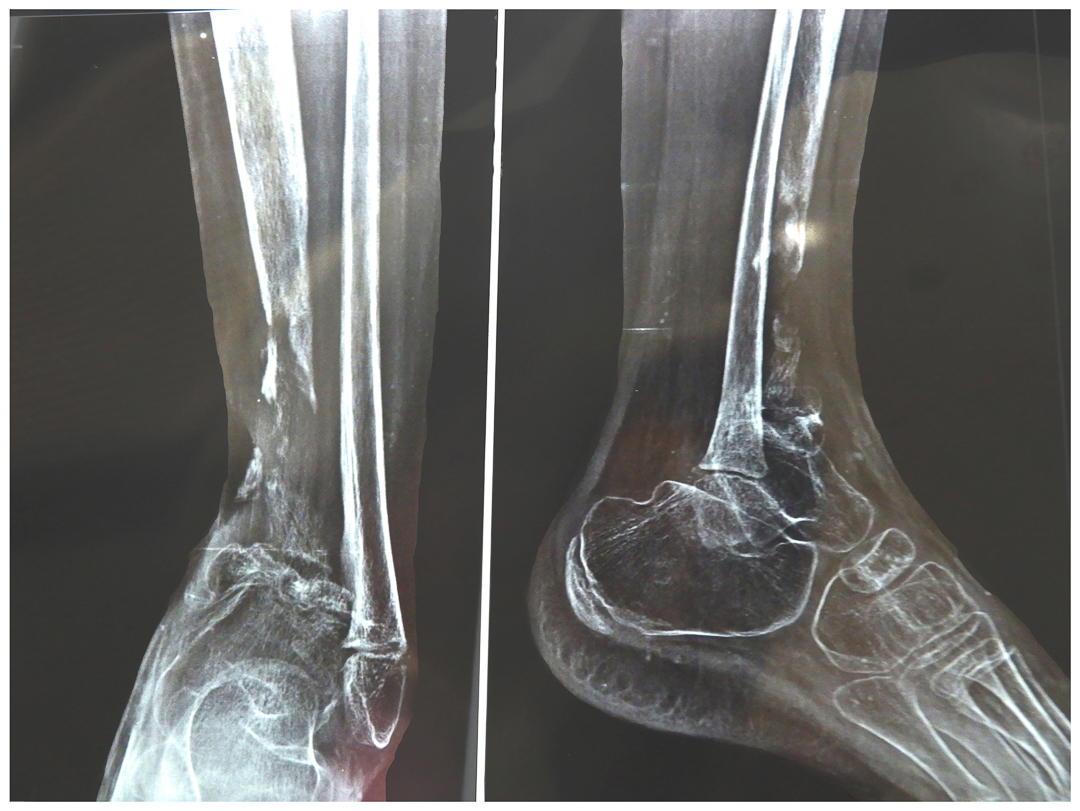
Before
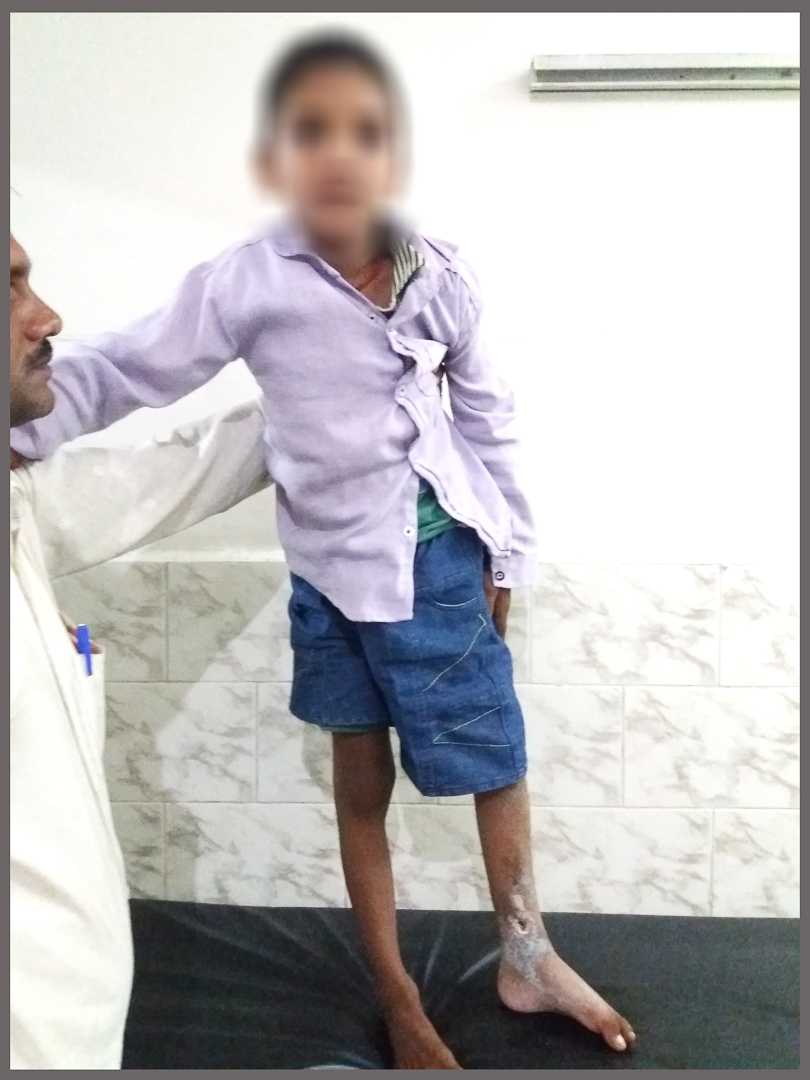
Before
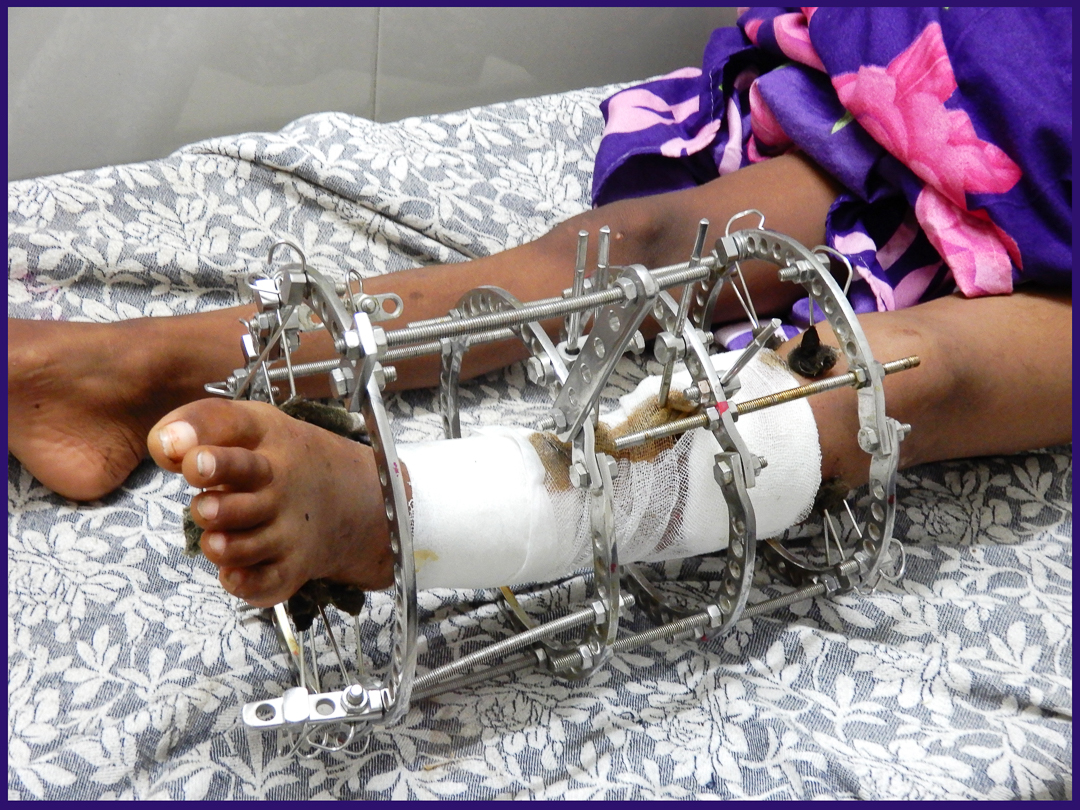
After
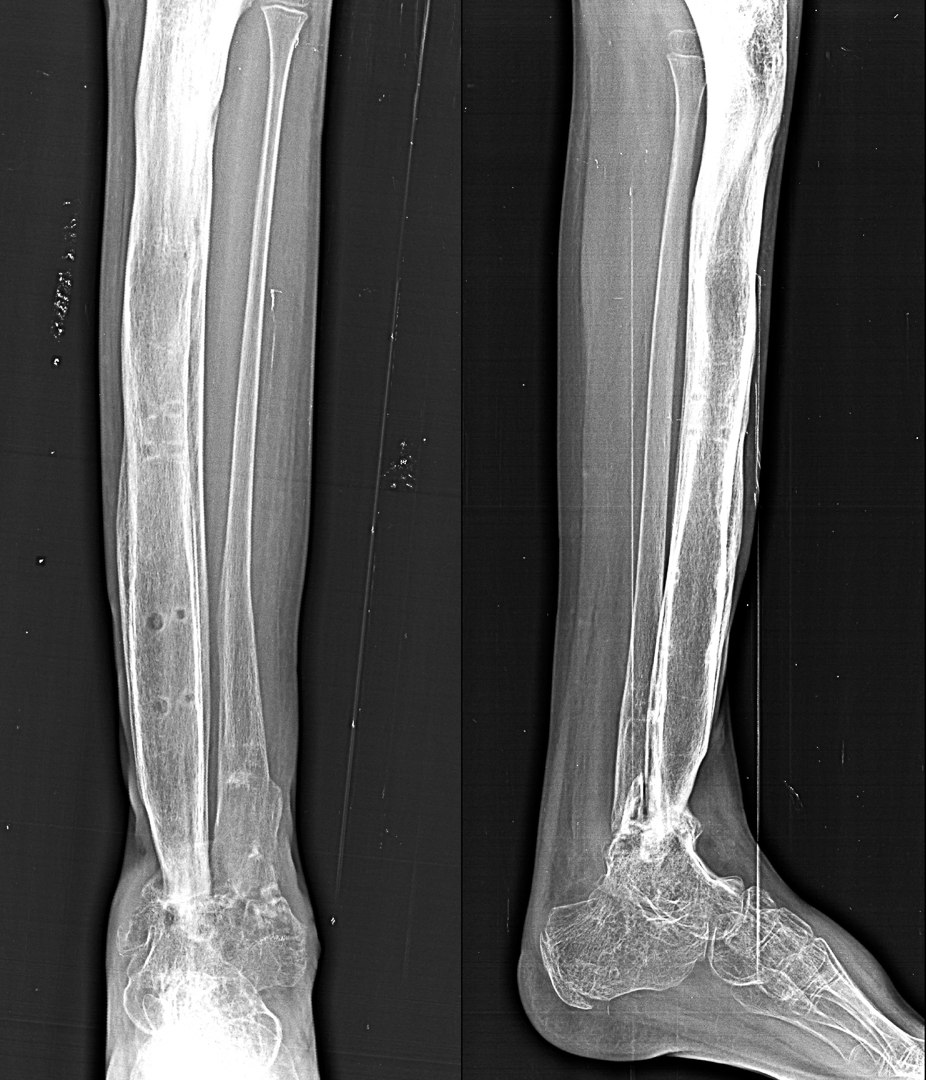
After
Perthes managed by proximal femur varus osteotomy
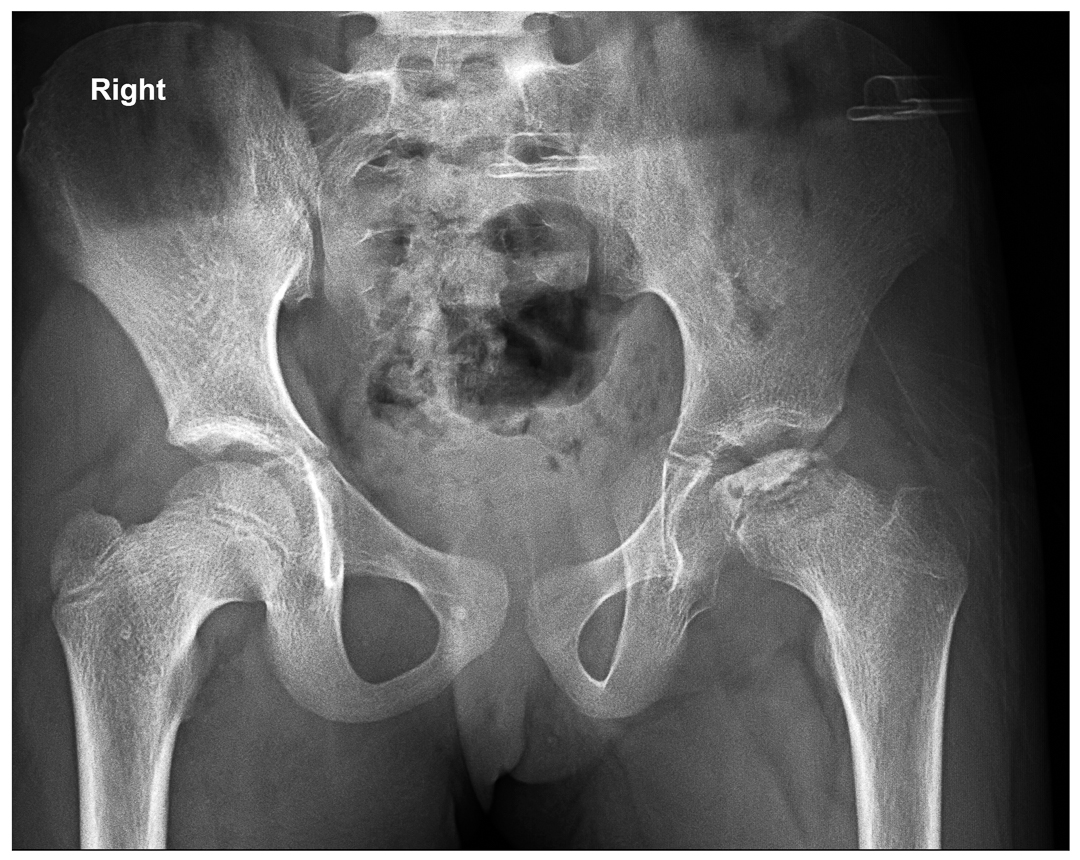
Before
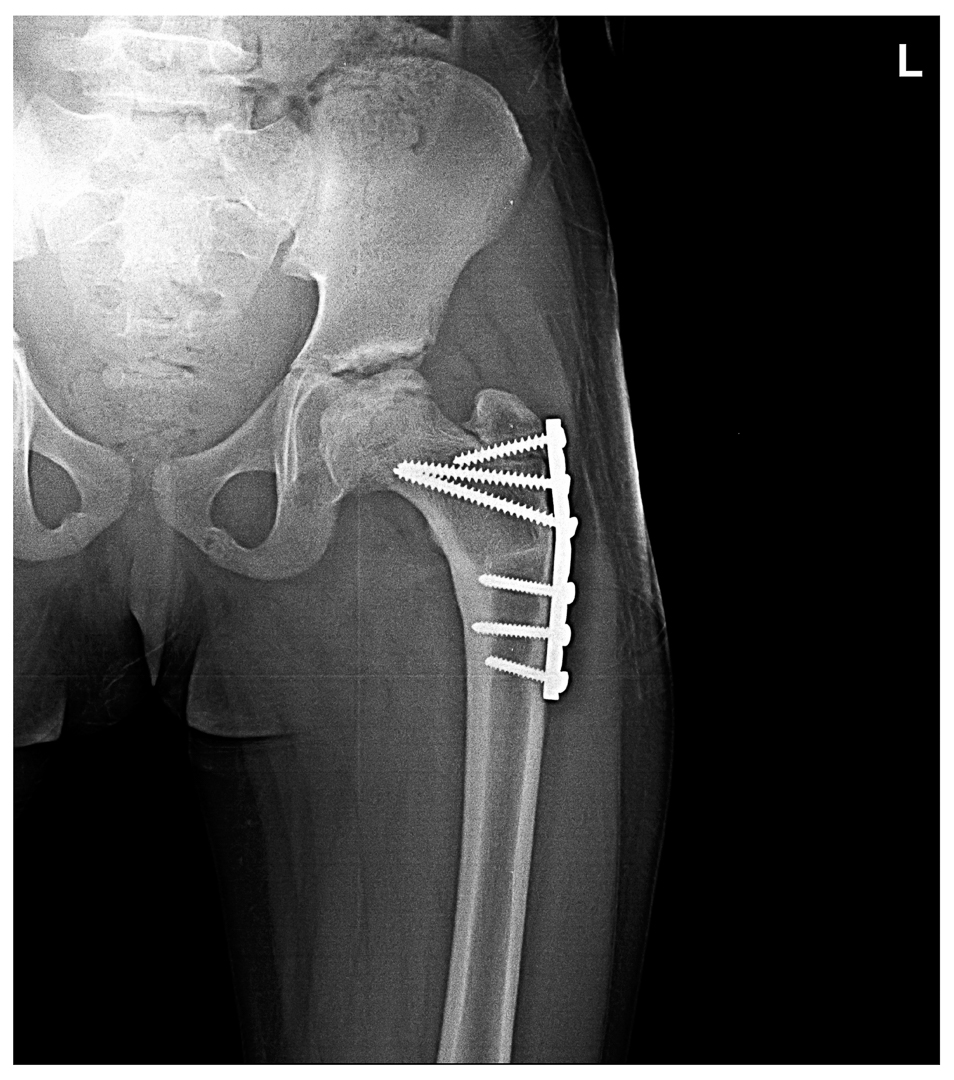
After
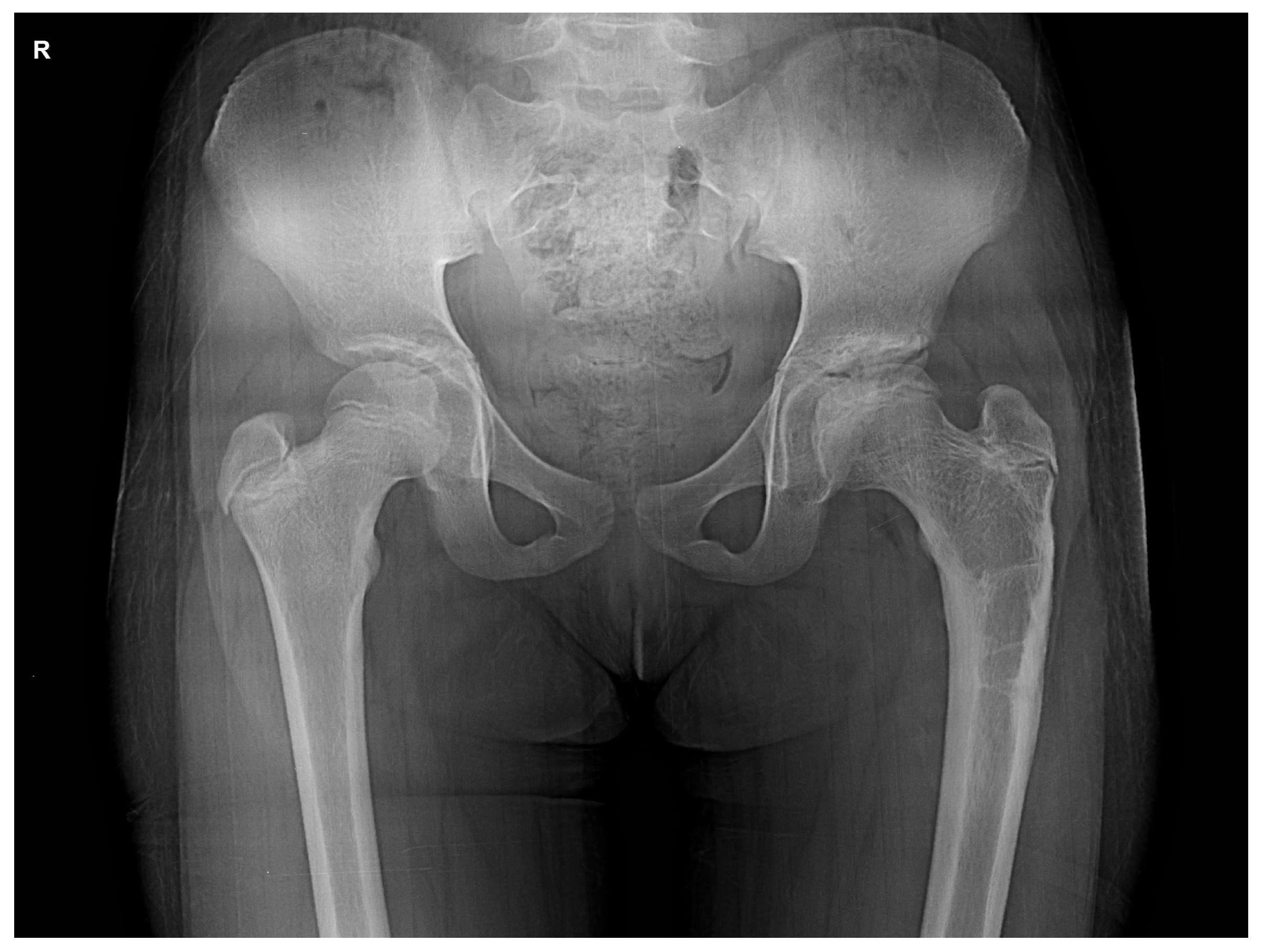
Final
Perthes managed by plaster in abduction

Before
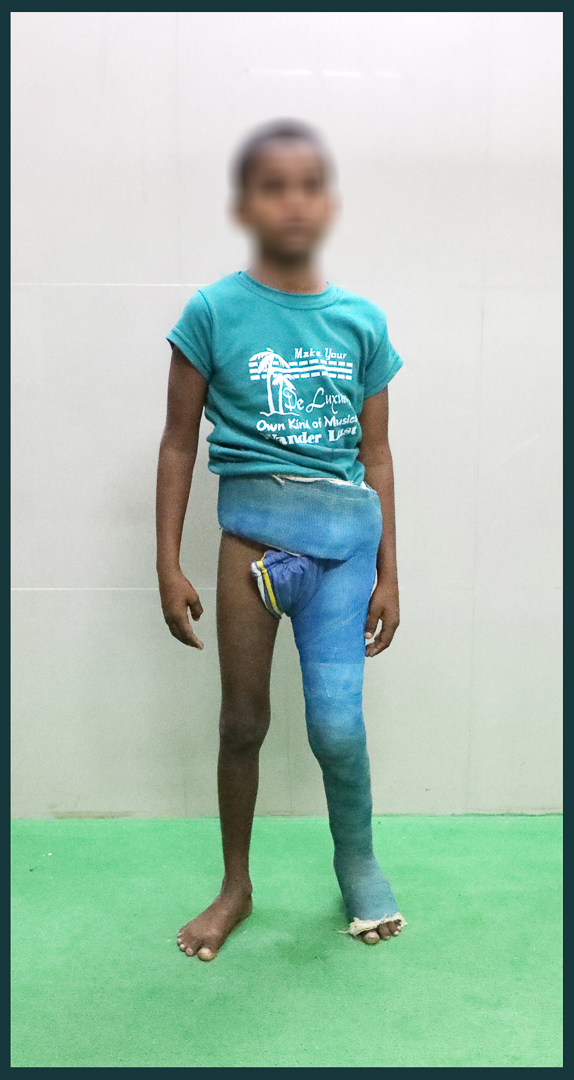
During Plaster
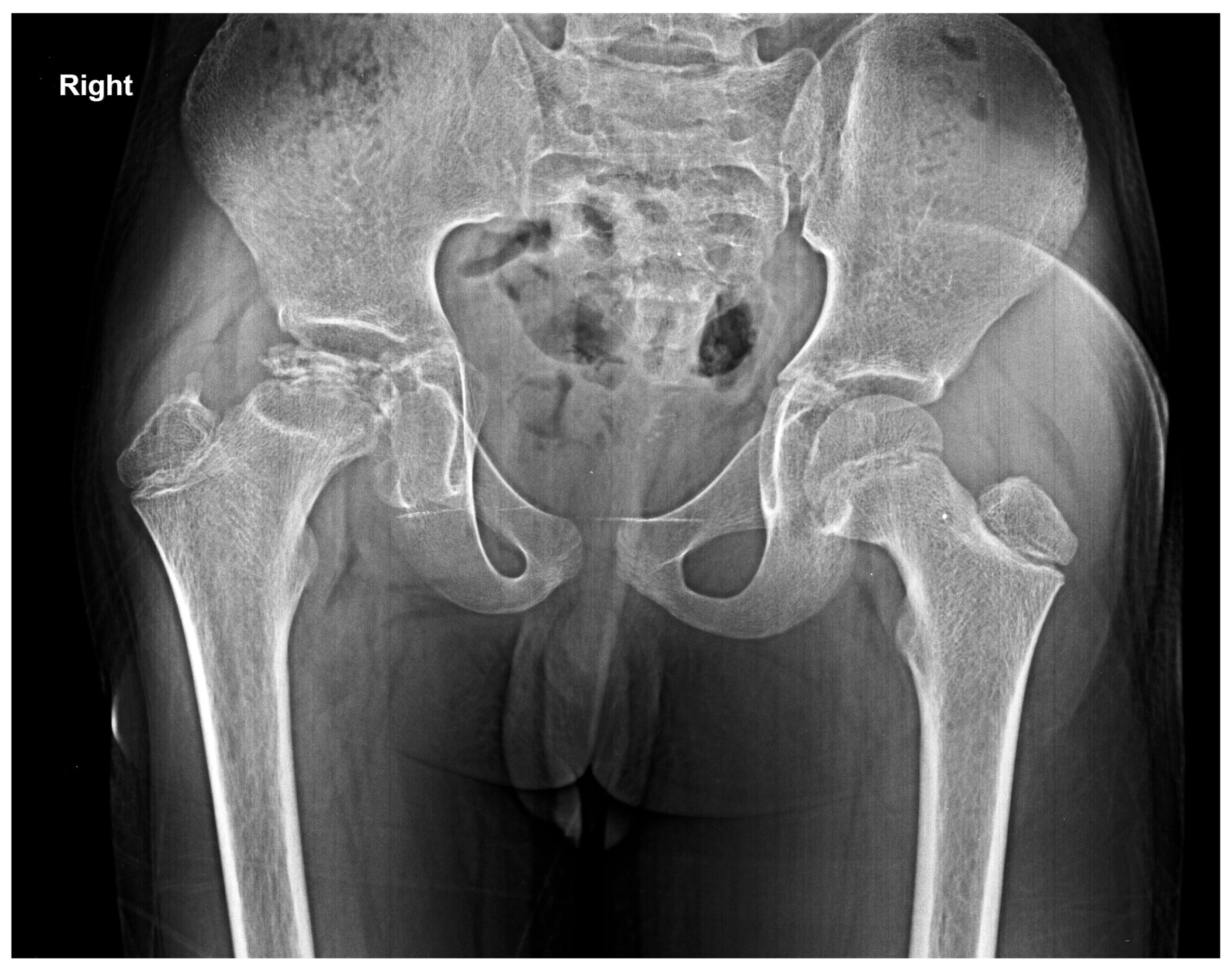
Final
Post polio deformity

Before
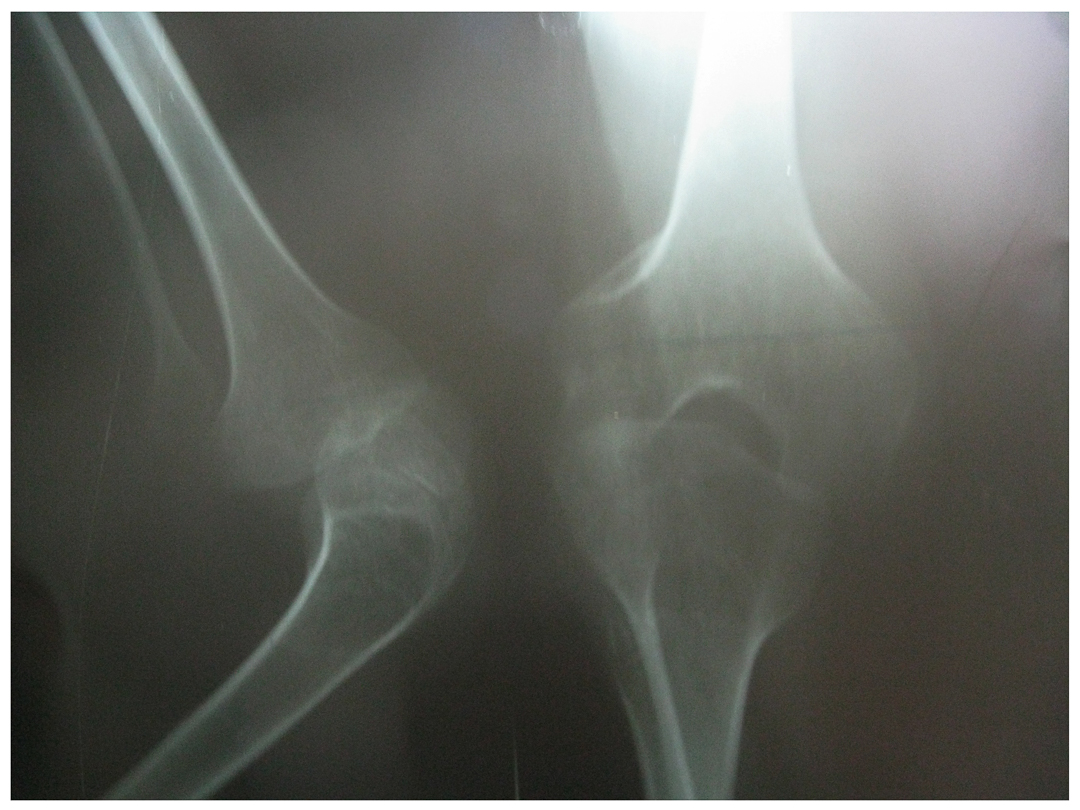
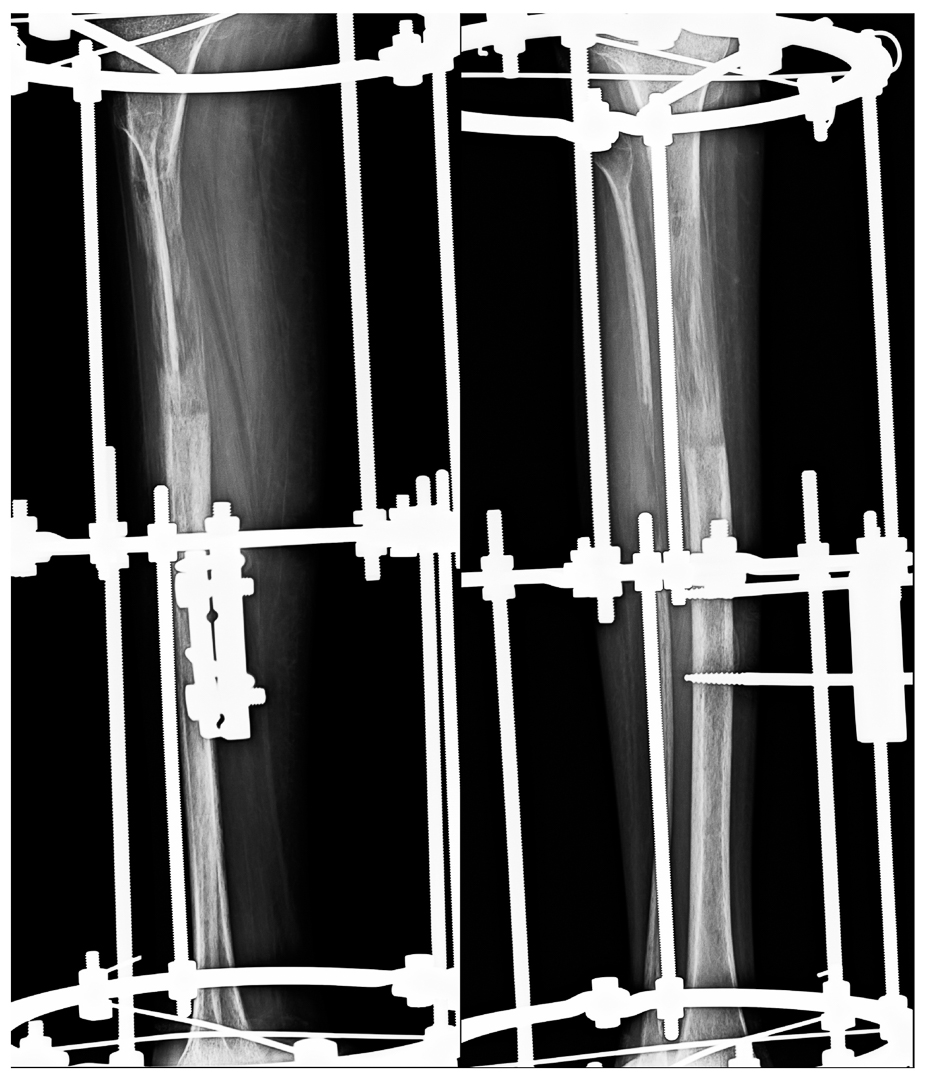
After Surgery

Torticolis

Before

After
Reviewed and Submitted by Dr. Jitendra Kumar Jain
Last updated on July 11, 2020
Dr.Jitendra Jain, MD and DNB (Orthopedics), president at Trishla Foundation, an NGO for treatment of cerebral palsy, and a Consultant Pediatric Orthopedic Surgeon & Cerebral Palsy Specialist at Trishla Orthopedic Clinic & Rehab Center.
Dr. J. K. Jain is a member of the general council at Dr. SMN university of rehabilitation, Lucknow, a member of the advisory board chief commissioner for PWD, Govt. of India (New Delhi), a member of the state disability research committee (U.P.), and a member of the committee of RCI, New Delhi. He has been awarded many awards, including the Dr.Bhagawan das memorial award, the spirit of humanity award, and the state govt. award for his services towards PWD, etc. Times of India has posted his work many times and mentioned him as one of the best doctors in the field of Pediatric Orthopedics. He helped many children recovering from cerebral palsy, just like comedian jay Chanikara, who is now able to stand and walk without any support, Abena, a Ghana girl with cerebral palsy, and many more. He also organized the National Wheelchair cricket tournament and created World’s first cerebral palsy village foundation in Prayagraj. He successfully treated 10,000+ children with various kinds of orthopedic disability, conducted 160+ free assessment camps, and produced a documentary film on cerebral palsy.
Walk in Appointments Available Daily
You can make an appointment online for video tale-consultation by fixing up an appointment at this website or you can visit the clinic to make an appointment in person and show to doctor with the care of social distancing at the given time.
Contact us
Call Us
0532-2468989
+ 91 9415014994
+ 91 8577873545
+ 91 9455001645
Email Us
totrishlaortho@gmail.com
Our Location
Dr. Jitendra Kumar Jain
Trishla Orthopedic Clinic & Rehab center, 182C / 350A, Tagore Town, Prayagraj (Allahabad) U.P-211002, India
